Several attempts have been made to classify HH in order to better understand the characteristics and the impact the HH may have on the surrounding critical structures in that area of the brain.
What type of HH you have will be a factor when deciding on a treatment plan.
To properly understand hypothalamic hamartomas, a distinction must first be made between the 2 different subtypes or classifications. They are: 1) intrahypothalamic (or sessile) and 2) parahypothalamic (or pedunculated).
1. Intrahypothalamic (Sessile)
The intrahypothalamic (or sessile) HH has a base of attachment within the third ventricle and can be either partial or complete. These lesions vary significantly in size but typically extend into the third ventricle itself and distort the surrounding anatomical structures, most importantly, the fornix or mammilary body. These structures are critical in the process of memory and behavior and therefore it is common for short-term memory and behavior disturbances to be evident. Sessile HH’s are most often associated with neurological issues and an initial presentation of gelastic seizures with a progression to other seizure types. Just under half of individuals with sessile HH’s will develop precocious puberty at some point in their lifetime. It is not unusual for children with this type of HH to experience a progressive decline in behavior, cognitive abilities, and social skills.
2. Parahypothalamic (Pedunculated)
The parahypothalamic (or pedunculated) HH is more often associated with precocious puberty and not usually associated with epilepsy or neurodevelopmental problems. Treatment for these types of lesions is usually aimed at controlling the effects of the sexual development (precocious puberty) and premature bone development. Most cases can be easily classified into one category or the other, but some combinations of the two do exist.
The figure shows a representation of the Delalande and Fohlen classification, which further breaks the HH classification into four total subtypes.
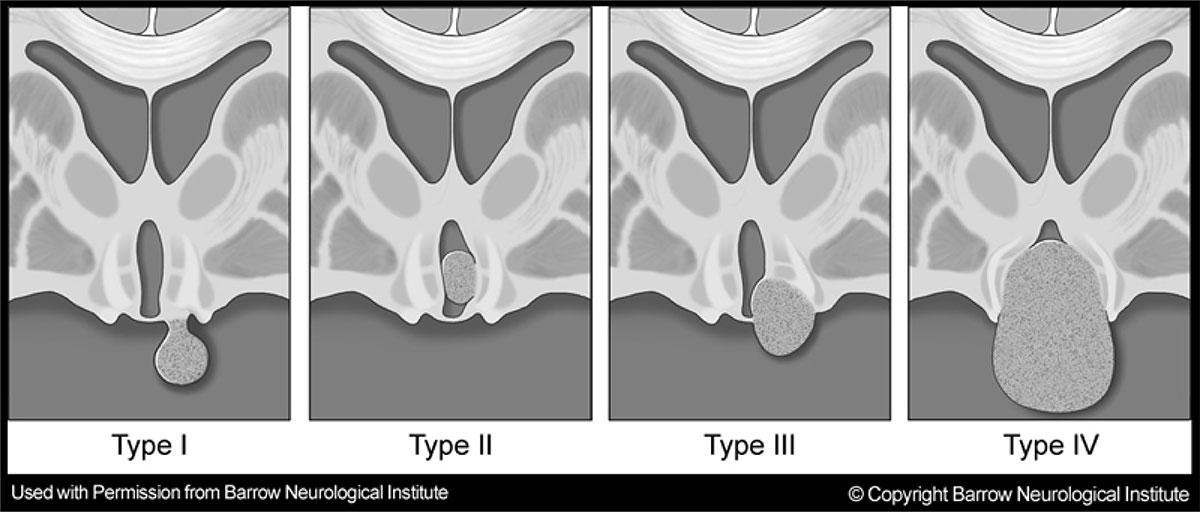
Type I:
These are HH lesions that attach below the floor of the third ventricle, with a horizontal plane of attachment to the underside of the hypothalamus. If these lesions have a narrow base of attachment in the anterior (most forward) region of the hypothalamus, they may be associated only with central precocious puberty, but a broader base of attachment, especially if it includes the more posterior portion of the hypothalamus, may have epilepsy and other neurological problems. Because of the site of attachment, these HH lesions are best approached surgically from below (that is, coming from below the temporal or frontal lobes).
Type II:
These are HH lesions that attach completely within the third ventricle (above the floor of the third ventricle), with a vertical plane of attachment. These HH lesions (and the ones that follow) are highly associated with epilepsy. Because of the vertical plane of attachment, and their often small size, this type is often ideal for endoscopic resection (or, if the patients is stable, gamma knife radiosurgery).
Type III:
These are HH lesions that attach both above and below the floor of the third ventricle (and, accordingly, have both vertical and horizontal planes of attachment). These lesions may be approached from above (either the open transcallosal approach or the endoscopic approach) or from below, or with a combination of the two. If the patient is stable, these type III lesions may also be treated with gamma knife radiosurgery.
Type IV:
These are defined as “giant” HH lesions by Delalande and Fohlen, although quantitative criteria for the exact meaning of “giant” were not suggested. Our group has used a volume of 8 or 10 cm3, depending upon the paper. These lesions are likely to be attached bilaterally to the hypothalamus, with planes of attachment both above and below the floor of the third ventricle.
