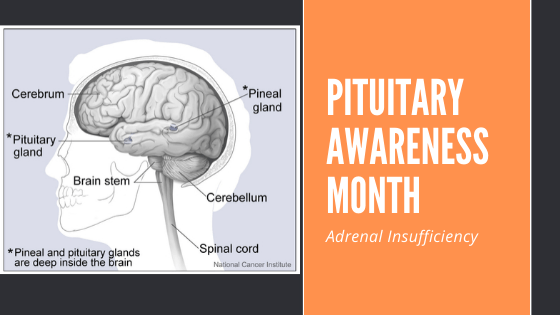
Pituitary Awareness Month – Adrenal Insufficiency
October is Pituitary Awareness Month – and you may be asking yourself “Why should I care if I, or my loved one, have an hypothalamic hamartoma (HH) and NOT a pituitary tumor?
Well, the hypothalamus is the master gland that feeds information to the pituitary gland, and when it is damaged, either by having an HH or as a result of surgery…many other hormones produced by the pituitary gland may be impacted! Several of these conditions will be all too familiar to some patients and/or caregivers, while some may want to explore the possibility of these being an undiagnosed issue for themselves or their loved ones. The general diagnosis for a deficiency associated with compromised pituitary function is called hypopituitarism. When more than one hormone is compromised, it is called panhypopituitarism.
Some of the more common conditions associated with both hypopituitarism and panhypopituitarism in HH patients include:
- Adrenal Insufficiency
- Growth Hormone Deficiency
- Hypothyroidism
- Diabetes Insipidus
- Low Sex Hormones (testosterone and estradiol)
In this blog series for October, we will be addressing some of the more challenging conditions and provide more background on treatments that are available today.
So, let’s get started with Adrenal Insufficiency.
Adrenal insufficiency is a condition in which the adrenal glands do not produce adequate amounts of steroid hormones, primarily cortisol; but may also include impaired production of aldosterone (a mineralocorticoid), which regulates sodium conservation, potassium secretion, and water retention.
For most individuals with HH, that also have issues with adrenal function due to injury to the hypothalamus, the resulting adrenal insufficiency is called secondary adrenal insufficiency. That means the condition was caused by an insult to the hypothalamus – most likely after surgery or radiation. When the hypothalamus is not making enough corticotropin-releasing hormone (CRH), then it affects the pituitary’s ability to produce adrenocorticotropin
(ACTH), in turn keeping the adrenal glands from producing enough cortisol.
Symptoms of adrenal insufficiency include fatigue, muscle weakness, low appetite, weight loss, and belly pain, among others.
Adrenal insufficiency can be difficult to diagnose. Tests that measure the levels of cortisol and aldosterone are used to make a definite diagnosis and include the following:
- ACTH Stimulation Test: This is the most specific test for diagnosing adrenal insufficiency. Blood cortisol levels are measured before and after a synthetic form of adrenocorticotrophic hormone (ACTH), a hormone secreted from the anterior pituitary, is given by injection.
- Insulin-Induced Hypoglycemia Test: The insulin-induced hypoglycemia test is used to determine how the hypothalamus, pituitary and adrenal glands respond to stress. During this test, blood is drawn to measure the blood glucose and cortisol levels, followed by an injection of fast-acting insulin. Blood glucose and cortisol levels are measured again 30, 45 and 90 minutes after the insulin injection. The normal response is for blood glucose levels to fall (this represents the stress) and cortisol levels to rise.
The treatment for adrenal insufficiency is typically hydrocortisone but prednisone may also be used.
It is important to understand that adrenal insufficiency can be life threatening if not monitored carefully. Adrenal crisis is a medical emergency and potentially life-threatening situation that can happen and requires immediate emergency treatment. It occurs when there is insufficient levels of cortisol in the body. This may be due to physical stress such as infection, dehydration, trauma, or surgery.
For a deeper dive into Adrenal Insufficiency, you can watch an excellent presentation by Dr Kevin Yuen, Adult Endocrinologist at Barrow Neurological Institute, Phoenix, AZ. Titled: Me, Myself and My Adrenal Insufficiency.
Adrenal Insufficiency in general can be a challenge to diagnose. Sometimes secondary diagnoses are harder for HH patients because treating an individual with a complex rare syndrome is hard enough! Surgery complications can make additional diagnoses even harder! Many of the conditions we will be discussing in this series of blogs occur together because they are the result of damage to the hypothalamus.
If you, or your loved one, have already been diagnosed with one of the conditions mentioned, it may be worth asking your endocrinologist about the possibility of other conditions being present. Many families have had to ask their endocrinologist, or more than one doctor, to do the proper tests to get the correct diagnosis!
For Family Support, some great resources include:
Magic Foundation – https://www.magicfoundation.org
Hormone Health Network – https://www.hormone.org/diseases-and-conditions/adrenal-fatigue
Join us next time for a discussion of Growth Hormone Deficiency!





